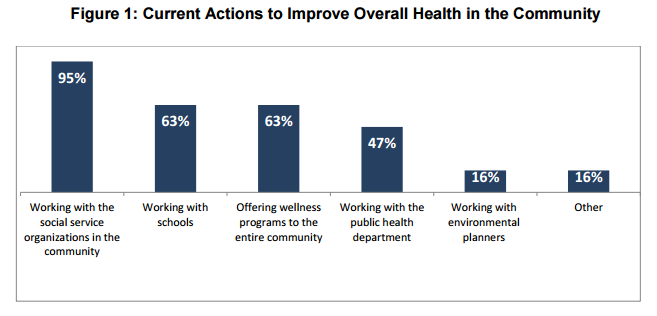
Accountable Care Organizations Expand Use of Social Services
New research shows that accountable care organizations are partnering with community resources and social service agencies to improve population health management.

- Today, accountable care organizations (ACOs) are focused on expanding their coordination efforts with social service agencies and community resources, according to findings from a report completed by the Premier Research Institute and the Robert Wood Johnson Foundation.

Private payers and the alternative payment models they’ve used among accountable care organizations have shown mixed results, but coordinating with social service agencies may bring improvements in population health management. Coordination with community centers will take the hospital-centered approach to healthcare in a significantly different direction, the report states.
Additionally, researchers from the Robert Wood Johnson Foundation interviewed leaders of accountable care organizations and found that more direction is needed from the multiple individuals that play a role in medical care including social service providers, clinicians, and the patients themselves. In particular, these groups will need to assess what still has to be achieved and how to best achieve the established goals.
The report also found that there are significant differences between payers and providers who were early adopters of accountable care organizations and those who were later adopters. The ACOs with less experience have been struggling to keep up their revenue and meet the quality benchmark requirements for the patient populations they serve.
The researchers used interviews and data from 19 accountable care organizations operating under Premier’s Population Health Management Collaborative to better understand where ACOs are struggling and identify remedies to any challenges, according to a company press release.
“Alternative payment models, such as ACOs, serve to shift the traditional fee-for-service model, which incents providers to do more rather than do better, to a value-based model that aligns incentives with measurable quality, cost and population health outcomes,” said Timothy Lowe, PhD, Director of Healthcare Research at the Premier Research Institute. “As providers develop and implement alternative payment models to align with value-based payment policies, such as the new Quality Payment Program for physicians, it is critical to identify what is working and what is not to support continuous change and improvement.”
Expanding their reach toward community service organizations and the patient community is expected to help accountable care organizations improve their population health management strategies.
The researchers found that ACOs have been working to provide transportation and modify patients’ homes to ensure their well-being. Some accountable care organizations have become the central arena where community service agencies have functioned through to reach patients in need of mental health assistance or drug dependency rehabilitation.
Along with these improvements, a number of accountable care organizations have started working with employers and local gyms to increase the amount of exercise employees pursue as well as provide nutritional information. Others have worked within the school system.
“Increasingly, providers understand how important the things that happen outside of the doctor’s office or hospital are to improving and managing a person’s health,” explained Andrea Ducas, Program Officer at the Robert Wood Johnson Foundation. “To that end, some leading ACOs are expanding their services to include more upstream, preventive support for patients and are also expanding their work to reach entire communities, rather than just focusing on their assigned beneficiaries.”
The researchers did find some of the obstacles standing in the way of accountable care organizations making a real connection with enhancing population health management. These challenges include inadequate staff funding, data system interoperability failures, physicians still working a fee-for-service mindset, and a missing connection among providers on the return of investment among population health management.
Some ACOs have also faced pressures from their payers. However, healthcare payers can work with accountable care organizations to address some of these challenges. Insurers could assist with improving interoperability of medical system technologies and educate clinicians on the benefits of alternative payment models.
When providers and accountable care organizations embrace the use of population health management and value-based care reimbursement, the quality of patient care can be improved while overall healthcare spending is likely to decrease. For example, one ACO, the Great Lakes Organized System of Care, has been able to reduce the rate of hospital readmissions and increase the number of cancer screenings through greater patient outreach.
By bringing more focus on value-based care and quality metrics, the accountable care organization also cut their rate of emergency room visits, said Lori Dale, Executive Director of Great Lakes Organized System of Care, in a prior interview.
“We look at value-based care in terms of cost and quality,” Dale said. “Since we’ve been focusing on our preventive testing to get patients in, we’ve seen significant increases in the number of cancer screenings and a decrease in our emergency room utilization. I pride our primary care practices on that. We focused on that two years ago.”
“It is really not good patient care to have them continue to go to the emergency room for things that are not emergent,” Dale explained. “We focused on how to keep our patients from going to the emergency room. Our physicians have extended their office hours so that patients could get in right away for urgent issues. Practices have worked hard at educating patients on the pitfalls of going to the emergency room when it’s not an emergency.”
Private payers may need to work with accountable care organizations to make more strides in population health management and bring community service organizations into the mix of advancing the quality of patient care.
Image Credits: Premier Research Institute
Dig Deeper:
Time, Commitment Required for ACO, Value-Based Care Success
What Are the Benefits of Accountable Care Organizations?