How Employers Can Design High-Quality Cancer Care Benefits
Cancer care can be costly and confusing for members of employer-sponsored insurance plans, prompting payers to offer enhanced care coordination and high-quality benefits.
Source: Thinkstock
- Designing meaningful and high-quality cancer care benefits is a challenge for employer-sponsored health plans.
Cancer, a costly and complex condition that takes many different forms, requires coordination across the entire healthcare continuum. Developing communication tools and financial support for plan members as they navigate their cancer care can help to improve outcomes and reduce anxiety for employees at a critical juncture in their healthcare journey.
The National Cancer Institute estimates that national spending on cancer care exceeded $147 billion in 2017. That number is likely to rise as more individuals are diagnosed with one of the many types of cancer.
In 2018, over 1.7 million new cases of cancer will be diagnosed, and 609,400 individuals will die from the disease.
Cancer diagnoses also create additional fear, stress, and confusion for plan members. Employees may require extensive communications from the health plan to determine the best course of action when diagnosed with cancer.
READ MORE: How Payer Philanthropy Can Address Social Determinants of Health
“Navigating [the complexity of cancer] calls for an approach that improves quality, manages cost and improves the employee experience,” NEGBH said.
“Consider this: employees may not even be aware that their company offers a range of cancer care services. After all, an employee handbook or benefits website isn’t the first place someone turns to after learning they might have cancer. That is a moment when they are afraid, stressed and overwhelmed. But that moment — just after a cancer diagnosis — is exactly when — if possible — the benefits department should get involved.”
Creating a coordinated cancer care team
Employers should consider aligning the health plan with benefit administrators and clinical care experts, NEGBH suggested.
Developing a coordinated care team for cancer patients can ensure communication across all parties involved in administration and clinical services. An ideal team leader would be a healthcare professional, such as a nurse or care coordinator, that has experience working with both health plans and benefit vendors and is comfortable coordinating activities across groups.
Other members of the team may include health plan experts, medical experts, oncology care case managers, pharmacy managers, and wellness coaches. The team leader guides and manages these participants to address both quality care and member engagement challenges.
READ MORE: Top 10 Highest Performing Medicare Advantage Health Plans
The care team should make sure to track important care quality milestones during the employee’s cancer care. Milestones include making sure patients know what their cancer care plan is, connecting the patient to the appropriate provider, managing medication side effects, and accommodating either a return to work or hospice care.
Quality milestones should be communicated to all participants to ensure effective collaboration.
Addressing clinical care for employees that need cancer treatments
An employee’s cancer benefit package should provide early cancer detection services as well as oncological treatments.
Employees that receive cancer screenings are more likely to detect cancer early, which can drastically improve their healthcare outcomes. NEGBH noted that the early detection of cancer allows the care coordination team to become involved before a patient’s cancer worsens. Early detection also leads to a higher chance of entering remission.
Early detection activities should be performed multiple times for employees at a higher risk for developing cancer. These screenings may help beneficiaries detect false positives - or false negatives - and improve decision-making.
READ MORE: Member Engagement, Medicare Advantage Growth Top 2018 Payer Trends
“It is very important that patients and families are confident in the diagnosis and able to choose from treatment options according to accurate information and preference,” NEGBH said.
Employees that receive a cancer diagnosis may require specialized benefits and care management for multiple conditions and side effects.
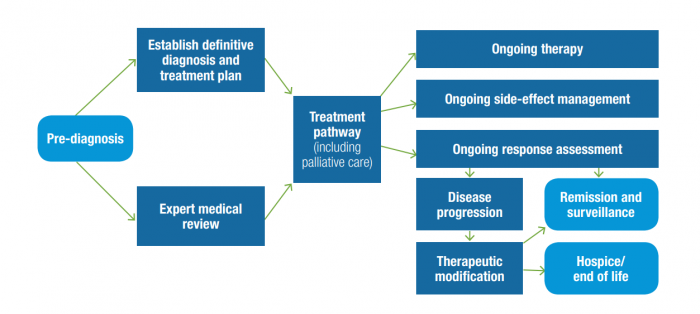
Source: NEGBH
An effective treatment plan should limit the impact of side effects on a patient’s quality of life, utilize an employee-focused treatment schedule to accommodate lifestyle needs, and consistently monitor patients during periods of remission.
Enhancing member engagement
Employer health plans may also want to revamp their member engagement capabilities so that members can understand how their health plan manages cancer care.
Employees should have up-to-date communication systems and engagement channels in place to understand how they can seek out care. These engagement channels include direct online chat lines with benefit coordinators, cancer benefit-specific educational programs, and wellness campaigns from patient coaches.
NEGBH also recommends incorporating benefits and support services such as subsidized medical transportation, disability care, life insurance, and financial advocacy services. These services are designed to help employees manage the stress and anxiety of their conditions.
Additionally, employers can improve cancer care engagement by developing cancer-specific online portals, so members can review their programs, policies, and guidance about available benefits.
NEGBH concluded that employer-sponsored health plans of all sizes can take immediate actions to address cancer care and cancer benefits administration challenges for their employees.
Employers can conduct internal reviews of claims data and communication channels to begin designing appropriate care benefits and developing member engagement platforms.
Employer-sponsored health plans should also initiate discussions with benefits vendors, clinical teams, and other professionals to develop a collaborative cancer care plan. Aligned cancer care coordination allows the health plan to implement an improved cancer care program at a faster rate.
“Providing support to an employee diagnosed with cancer is very complex,” NEGBH said.
“The clinical experience must be managed, and employee benefits must be coordinated. An employer must also account for the heavy emotional and social toll of cancer and the disruption it can bring to home and work life. One vehicle for doing so is the creation of a cancer care-focused team. But whether you decide on a huddle or another approach, what’s important is that the employee is placed at the center so that their experience is as positive as it can be, given what they are facing.”
