Integrated Medical, Pharmacy Benefits Help Costs, Member Engagement
Integrating medical and pharmacy benefits gives payers more visibility into member activities, which can cut costs and improve outcomes.

Source: Thinkstock
- Integrating medical benefits with pharmacy benefits can help healthcare payers and employer sponsors lower spending, improve member engagement, raise satisfaction, increase care coordination, and manage population health – ticking all the boxes for value-based care.
The increased engagement and reduction in health spending stemming from synthesized medical and pharmacy benefits can save hundreds of dollars per patient, industry research shows, by helping individuals achieve control of their chronic diseases and simplify the process of navigating the complex healthcare continuum.
A recent study released by Cigna shows that integrated medical and pharmacy benefits is helping save an average of $253 annually for employers by bolstering member self-management and giving payers a more comprehensive insight into utilization rates.
Cohesive benefit design created a 12 percent bump in the number of individuals participating in health coaching and case management program, as well as a similar rise in the number of beneficiaries undertaking healthcare improvement activities.
“Every time a prescription is filled, there is an underlying medical issue,” noted Scott Josephs, MD, Cigna national medical officer. “A real-time view of our customers’ health needs across both their pharmacy and medical benefits enables us to more easily identify and support those who need help in managing their health.”
READ MORE: Employer Health Plans Can Engage Members with Data, Targeting
“We’re able to provide personalized guidance to customers on actions that will drive better health – such as improving adherence to their medications – and provide cost savings for them and their employers.”
Patients with certain chronic diseases saw even higher savings, the study added. Streamlined benefits management contributed to an annual average savings of $2816 for diabetes patients.
“Even the best doctors and most effective medicines can only do so much if patients are not also actively involved in improving their health,” said Jon Maesner, PharmD, Cigna chief pharmacy officer.
“Under the plans we administer, pharmacy is the most frequently used benefit, and we use those touchpoints to encourage customers to participate in programs available across their benefits. The study helps confirm the added value we can provide to customers and clients when we are able to use this connected approach.”
Cigna isn’t the only payer touting the benefits of bringing both sides of the equation under one entity’s control. Aetna conducted a similar analysis earlier in 2017, and found equally promising results.
READ MORE: 44% of Employees Don’t Know Value of Health Plan Benefits
Members with six of the highest-cost chronic diseases, including diabetes, arthritis, HIV, hypertension, coronary artery disease (CAD), and chronic heart failure realized a decrease in medical spending that ranged from 2 to 17 percent under an integrated medical-pharmacy benefit plan.
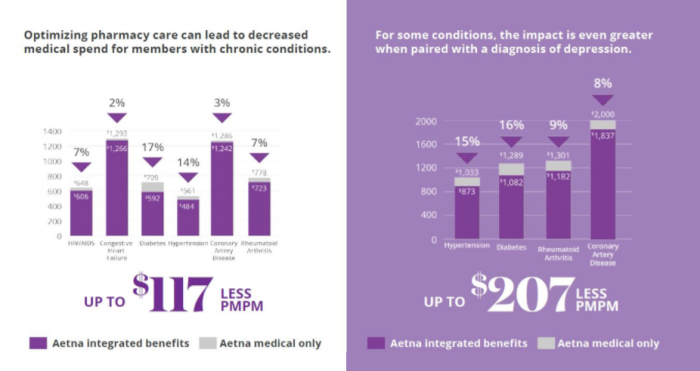
Source: Aetna
These patients experienced fewer hospital admissions, fewer days in the hospital when an admission was required, and fewer emergency department visits, which contributed to the reductions in spending.
For patients experiencing certain high-cost chronic diseases alongside a diagnosis of depression, the savings were even higher. Savings for patients with depression and coronary artery disease were five percent higher than the savings for CAD alone, Aetna says.
While Cigna saw some modest increases in member engagement, Aetna says that members with the aforementioned chronic conditions are between 48 and 116 percent more likely to participate in care management programs when their benefits are aligned.
Members in need of high-cost services like infusion drugs were 63 percent more likely to be directed to a lower-cost care site than those with separate benefits packages, the study added.
READ MORE: Top 4 Consumer Wellness Benefits for Payers to Add to Health Plans
Adding more touch points to the member management process by folding in pharmacy benefits allows payers to offer low-cost, high-impact services like home delivery of medications and counseling from pharmacists.
Pharmacy-based interventions, including medication reconciliation and synchronized pick-up dates, have been shown to increase medication adherence, reduce patient safety risks, and help patients better manage their own health.
And when members are aware that they can turn to their payer to answer questions about their medications as well as their clinical care, they are more likely to be receptive to engaging with resources that can address all of their concerns, says Michelle Vancura, Senior VP of Sales and Clinical Account Manager for Cigna Pharmacy Management.
“Cigna’s data finds that 70 percent of individuals who are inquiring about their medications and are invited to work with a health coach agree to be transferred to that coach in real time,” she wrote in a 2017 issue of Benefits Quarterly. “Of these, more than 90 percent go on to demonstrate progress towards their goals.”
For payers, the benefits of bringing medical and pharmacy benefits under the same roof are manifold. In addition to fostering better health for patients and lower subsequent spending, payers can control costs on the back-end, as well, by encouraging the use of generics and gaining more negotiating power with pharmaceutical manufacturers.
Payers may even be able to make headway against the expanding epidemic of opioid abuse, suggests Vancura.
“Integrated analytics help detect opioid use patterns that suggest possible misuse by individuals,” she explains/ “A benefits administrator can then alert what may be multiple health care providers for one patient to this possibility, so that individuals who do have substance use disorders can be identified more quickly and get the help they need.”
This added visibility into a patient’s activities, especially for complex chronic disease patients, is one of the primary benefits of integrating both types of benefits, Vancura notes, and may produce even higher savings and better outcomes than currently envisioned.
“The advantages of pharmacy benefit integration go well beyond the convenience and efficiency of having a single point of contact for both plan sponsors and employees,” she said. “The value lies in having a comprehensive understanding of an individual’s health journey and making those care connections easier and more effective along the way.”
