Population Health Management Achieved through Accountable Care
Medicaid Accountable Care Organizations are proving to be an excellent way to fuse both healthcare payment reform and population health management.

- Population health management is a complex area within the healthcare industry that has received a much bigger spotlight in recent years. In particular, after the Patient Protection and Affordable Care Act became law, Accountable Care Organizations became a method for strengthening population health management strategies.

According to a brief from the Center for Health Care Strategies and the Urban Health Research and Practice at Northeastern University, ensuring better health outcomes and quality medical services is dependent upon effective population health management.
More traditional fee-for-service payment models have not assisted medical providers in boosting population health strategies, but new alternative reimbursement methods such as bundled payments and the Shared Savings Program could offer new pathways for improving public health outcomes.
Specifically, Medicaid Accountable Care Organizations are proving to be an excellent way to fuse both healthcare payment reform and population health management. The reasoning behind this is due to a focus on disease prevention and promotion of general wellness.
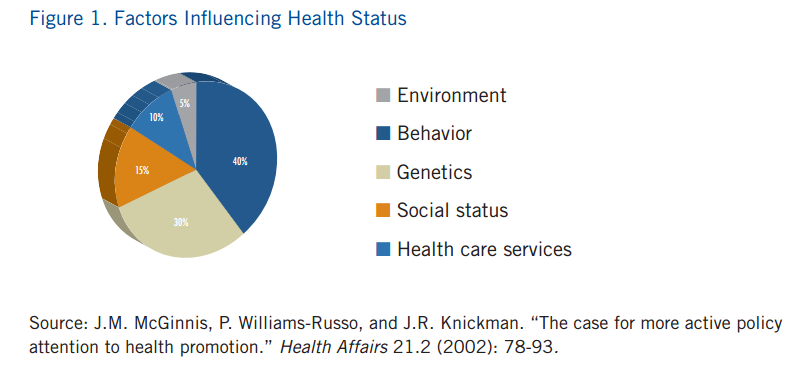
Research shows that the majority of preventable deaths are due to genetic factors, social situations, behavior, and environmental aspects. However, once the Affordable Care Act was passed, the healthcare industry was forced to look at how value-based care, new payment models, and ACO arrangements brought better public health outcomes.
From bundled payments and shared savings to pay-for-performance strategies, more providers and employers are focused on improving wellness and disease prevention through social programs. These initiatives are meant to reduce the number of hospitalizations and severe medical conditions like heart disease or diabetes across the nation.
Medicaid ACOs take on the responsibility of coordinating care for a certain population of patients among a variety of medical providers. Additionally, these particular organizations use financial incentives to support value of care instead of volume of services offered.
Medicaid ACOs use data sharing and integration, which are key in population health management, while at the same time, remaining accountable for quality measures. Since early 2015, there have been a total of 15 state Medicaid programs that have been actively managing an ACO.
“The opportunity for Medicaid ACOs to produce positive individual- and community-level results is promising, as Medicaid beneficiaries tend to have poorer health outcomes and greater social needs than higher-income populations,” the brief stated.
“In other words, individuals with Medicaid may have the most to gain from a health delivery system that focuses on keeping people healthy. States that have expanded Medicaid to cover all individuals up to 138 percent of the Federal Poverty Level have an especially strong incentive to incorporate population health improvement goals into payment and delivery system reforms.”
“States that prioritize population health in Medicaid ACOs should seek to align their efforts with non-Medicaid population health initiatives in their states and nationally. As a starting place, Medicaid leaders can form alliances with their public health and social services counterparts to achieve a unified population health strategy.”
As previously reported, commercial insurers are lining up alongside Medicaid and Medicare programs in implementing value-based care payments, which includes partnering with hospitals participating in Accountable Care Organizations.
Among three case studies outlined by the Commonwealth Fund, the biggest ways to improve population health management was illustrated through patient and family engagement strategies, care management among chronic medical conditions, and better care coordination among multiple providers.
Additionally, improving data analytics among each ACO was shown to strengthen care coordination. For example, one provider had an alert system that would warn physicians about any potential health concerns among patients. This alert system would help providers keep patients out of the hospital and thereby lower costs.
The Medicare Shared Savings Program is a major incentive for participating in Accountable Care Organizations (ACOs), as it would allow ACOs to share in up to 50 percent of their cost savings if the quality performance standards are met and the minimum savings rate is achieved.
Health Affairs reported on how population health management and accountable care are dependent upon physician leadership. One survey showed that physicians are showing significant interest in leadership roles among ACOs. However, there have been certain challenges such as hospital physicians not having trust in executive leadership of population health management programs.
One way to overcome some obstacles surrounding accountable care and physician leadership is to incorporate the Population Health Services Organization, which keeps a staff dedicated to the technology platforms and healthcare delivery models that will help population health to prosper.
One vital factor of the Population Health Services Organization is that it is physician-led, which will clearly boost leadership roles among doctors working directly with patients via accountable care arrangements.
“Through the structure of the PHSO, physician participation is integral in the ongoing development of the vision and strategy of population health programs. In addition to serving as champions of change management efforts, physicians are responsible for selecting clinical performance initiatives, standards of care, guidelines, and population health interventions,” Health Affairs reported.
Essentially, physician participation is a major factor for ensuring population health management is effective within an accountable care setting. With strong leadership and a team-based environment, ACOs can lead toward better public health outcomes around the country.