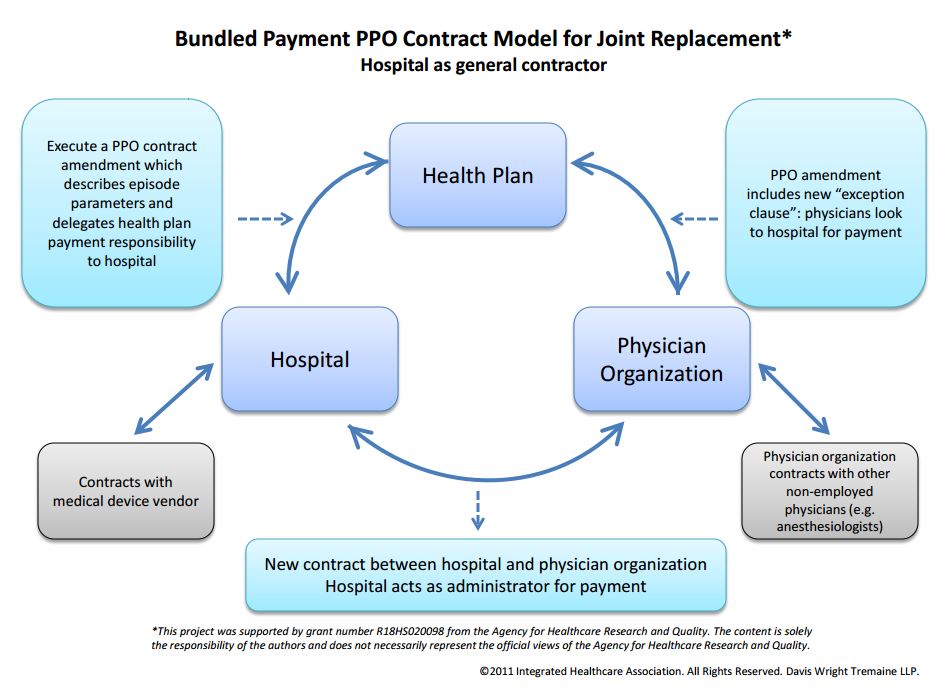
Top 4 Factors Necessary for Bundled Payment Model Contract
Risk-contracting is meant to stimulate healthcare providers to lower their overall spending. Additionally, when payers contract through a bundled payment model, they must define an episode of care.

- In today’s healthcare climate, payers are working to develop value-based reimbursement contracts with their provider network. Lately, payer and provider contract negotiations are often based around alternative payment methods such as the bundled payment model.

As previously reported, when payers and providers come to contract terms, they must first establish which medical condition will be bundled. It is especially useful when a particular condition has a specified cycle of care and is well-defined in the clinical sense.
Also, the two parties must determine the specific population that will be used in the bundled payment model as well as the health outcomes expected. Another important step is to fix the prices within the bundled payment contract and improve patient engagement in their overall care.
Types of bundled payment contracts
Sometimes payers work with large organizations such as a patient-centered medical home or Accountable Care Organization using a bundled payment model and then reimburse the entire medical entity, which allows the facility to reimburse individual doctors, nurses, and specialists. Another option is virtual bundling where payers reimburse every doctor and healthcare provider based upon previously agreed-upon negotiated contract rules.
When contracting through the bundled payment model, payers and providers should also be aware of risk-contracting, which consists of providers losing any extra costs of their services that go beyond the agreed-upon bundled reimbursement amount.
Risk-contracting is meant to stimulate healthcare providers to lower their overall spending. Additionally, when payers contract through a bundled payment model, they must define an episode of care and the duration of the contract agreement.
Early steps toward bundled reimbursement
A paper from the Harvard Business School establishes that bundled payments are a surefire way of bringing providers, suppliers, and payers to focus on patient value. Bundled payments force providers to improve health outcomes for the patient and bears them responsible for any costs beyond agreed-upon care such as in the case of avoidable complications.
Recently, a number of large employers and corporations such as Walmart, Lowes, and Boeing have used bundled payment contract with healthcare providers when offering healthcare services to employees who need specific medical treatments such as cardiac surgery.
The Affordable Care Act further pushes payers and providers to embrace the bundled payment model and other steps to reduce healthcare costs.
“Traditional American healthcare is inefficient and wasteful. Costs vary enormously from provider to provider—sometimes by an order of magnitude—and until recently were largely opaque… Under the ‘fee-for-service’ system every blood test, bandage or X-ray triggers a payment,” The Economist reported.
“Obamacare introduced (or encouraged the adoption of) various tools to restrain all this. For example, health-care providers receive financial rewards for cutting costs and penalties for bad care, such as when patients have to be readmitted to hospital after they have been discharged or when they catch nasty infections in a clinic. Between January 2012 and December 2013 there have been 150,000 fewer readmissions among Medicare patients—an 8 percent decline.”
“The health law encourages the use of ‘bundled payments,’ where a hip replacement or a heart bypass generates a single fee, no matter how many tests are performed or how many complications arise.”
However, there may not be enough detail and background for developing an effective risk-based bundled payment system and create a real value-based care reimbursement platform within the federal legislation, according to the Harvard Business School paper.
Four essential ingredients for bundled payments
The Harvard Business School paper outlines four necessary components for a value-based bundled payment system. These elements include: (1) healthcare coverage for a specific medical condition, (2) basis on risk-adjusted health outcomes, especially those important to the patient population, (3) payment is tied to effective and efficient care, and (4) limits are made regarding costs and care for unrelated patient needs and “catastrophic events.”
When looking to treat a specific medical condition, bundled payments are meant to cover all of the diagnostic tests, drugs, materials, and services a patient receives during a specific cycle of care.
The cycle of care could include the initial doctor visit for the condition all the way through “recovery and rehabilitation,” the Harvard Business Review paper states. When it comes to meeting risk-adjusted outcomes, providers are essentially tied to meeting quality performance measures and payments are based on the patient outcomes achieved.
Risk factors are taken into account when targeting the payment amount regarding these health outcomes. Payers will need to ensure that providers report outcomes before receiving their reimbursement.
Efficient clinical processes and administrative management is expected when contracting through a bundled payment model. Time driven activity‐based costing will need to be used to determine the full costs of treating a specific medical condition and thereby determine what costs should be contracted through a bundled payment system.
Finally, providers using bundled reimbursement contracts should be required to cover any of the costs that go beyond treating the particular disease or condition such as emergency care or a potential complication.
By integrating these four essential ingredients, payers and providers will be able to create an effective bundled payment contract and potentially improve the quality of care across their facility.
“Past barriers to adoption of value‐based bundled payments are being overcome. Providers are organizing care around integrated practice units, outcome measurement is growing rapidly, the tools to measure costs accurately for each medical condition are available, and consolidation of redundant care 20 is underway,” the Harvard Business School paper concluded.
“Much work remains to put these innovations into wide‐spread practice, but we are finally moving down the path of paying the right way for the right kind of health care.”