UnitedHealth Adopts Bundled Payment Model for Orthopedic Care
To reduce the high spend associated with hip, knee, and spine surgeries, UnitedHealthcare has adopted a bundled payment model.
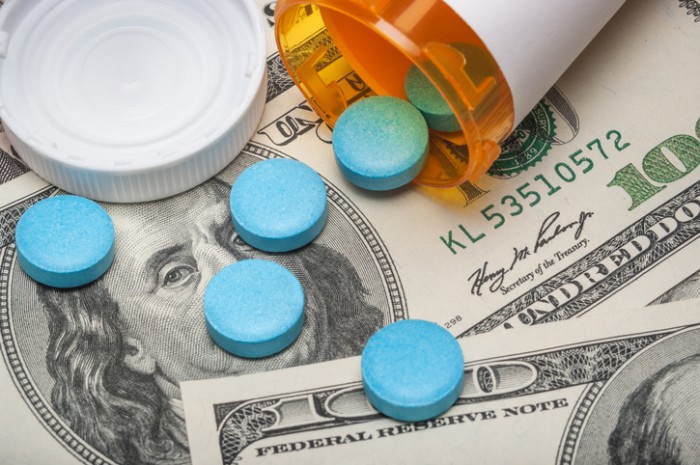
- Healthcare payers are finding that their reimbursement totals show higher spend for hip, knee, and spine surgeries and other orthopedic care when compared to other forms of treatment. Along with the higher spend, members regularly show poor health outcomes, said Michelle Lobe, Vice President of Network Strategy and Innovation at UnitedHealthcare. To counter these problems, UnitedHealthcare announced this month in a press release its new prospective bundled payment model for hip, knee, and spine surgeries.
“The main reason for developing a [bundled payment] program is that, in most large companies, high spend is really associated with orthopedic procedures,” Lobe told HealthPayerIntelligence.com. “For the most part, about 17 percent of company spend is in the orthopedic arena. Hip, knee, and spine procedures constitute about 33 percent of that.”
“Many companies are looking for ways to streamline payment and provide quality centers for their members to have more efficient, high-quality surgery,” Lobe continued. “That was the birth of why we focused on Centers of Excellence for spine and joint surgery.”
With 17 percent of all healthcare spending based on treating musculoskeletal conditions and 33 percent for hip, knee, or spine treatment, “to put a real number on that, 17 percent of average healthcare spend is about $45 dollars per member per month. That’s real cost for a company,” said Dr. Jon R. Friedman, Chief Medical Officer of Complex Medical Conditions at Optum.
With a large percentage of payer reimbursement based in orthopedic care, health insurance companies that implement bundled payment models and partner with high-quality providers may see a decrease in cost for orthopedic surgeries. The decrease in cost may be related to members spending fewer days in the hospital and stronger population health results, said Lobe.

Bundled payment models would be a beneficial solution for cutting costs. Bundles hold healthcare providers accountable for quality of care and patient safety. For instance, providers looking to boost their revenue would be incentivized through a bundle to ensure fewer costly hospital-acquired infections.
By partnering with high quality providers, payers may also find their members experience better outcomes and decreased cost, the UnitedHealthcare press release stated.
One of the potential challenges of adopting bundled payment models involves becoming knowledgeable about a new payment structure. Since bundled payment models differ greatly from traditional fee-for-service reimbursement systems, payers and providers may need more time to become capable in the new payment structure.
“There are challenges in that this is a new payment methodology. Prospective bundles are different in the way Medicare participates and pays bundles on a retrospective basis. The facilities and the physicians that we’re working with to create the bundle, they need to have the capability to administer that,” Lobe explained. “If we pay the bundle to a facility, they need to be able in turn to reimburse the anesthesiologist, the surgeon, or any other professional associated with that hospitalization.”
To reduce the higher spend and poor outcomes of orthopedic surgeries, payers will need to move beyond merely creating bundled payment contracts with their provider network.
The first steps payers should take is to partner with high quality providers and target markets to find quality facilities. Lobe also recommends payers to use data analytics to pick the right partners and include CMS health outcomes and quality data. Once the right partner is picked, then payers can begin negotiating prospective bundled payment contracts.
“The first step is to go through some very specific analytics in the markets that we’re targeting to determine which the right center of excellence might be,” Lobe continued. “Before we get into any conversation about payment methodology, we’re looking first to find the highest quality centers to target for those discussions.”
“Using our own data as well as CMS data, we analyze centers for their outcomes and pick those partners,” she said. “Once we identify in a market which center of excellence might be a good partner, then we start to entertain the conversation about negotiating a prospective bundle.”
Lobe also discussed some other value-based care programs that UnitedHealthcare took part in such as payment contracts based on performance, bundled payment models in cancer care, and accountable care organizations (ACOs).
“We have a number of value-based programs all along a continuum starting with the performance-based program where we contract with our hospitals and physician groups and set quality targets for performance,” Lobe explained. “We have moved into different types of value-based programs. Bundles are becoming much more popular.”
“We have an episode of care payment program related to cancer care. We also have accountable care organizations. Some are shared risk arrangements and some are shared savings arrangements,” she pointed out.
Some of the outcomes from UnitedHealthcare’s value-based care programs include reductions in length of hospital stays, lower readmission rates, and better results in clinical quality improvement measures.
Lobe mentioned that accountable care organizations bring a greater focus on population health management. Friedman said that patients served in value-based care programs tend to have high member satisfaction upwards of 95 percent.
“There’s very good member satisfaction with this program,” Friedman added. “Upwards of 95 percent of members have been very satisfied with this program. The ease of what this does for the patient in a single bundled payment to the hospital brings a reduction of multiple surgical balanced bills from your anesthesiologist, radiologist, surgeon, and everyone else. It’s a seamless process for the member and brings very high satisfaction.”
The general advice the experts provided encourage payers to pick the right partners especially those facilities that want to pursue value-based care reimbursement. Payers will need to partner with providers looking to work in new payment structures and share clinical data.
“Bundles are a great way to provide employers with the predictability they’re looking for in pricing,” Lobe said. “It allows members to be more satisfied in terms of their outcomes and streamlines some of the paper processes and bills. It also gives providers the opportunity to share in the risk and gain.”
“For other health plans and payers, my advice would be to really pick partners who are very interested in value-based programs and collaboration because these programs are not easy to stand up. You really have to have a good partner very willing to work with you on new payment methodology and data sharing,” Lobe concluded.
Dig Deeper:
How to Overcome the Challenges of Bundled Payment Models
Key Steps for Payer Success in Accountable Care Organizations
