How to Design and Support an Accountable Care Organization
In order for an Accountable Care Organization to be successful, there will need to be strong leadership with a new vision and superior management skills.

- When a large establishment wants to bring more care coordination and greater organization among multiple medical facilities including primary care offices, hospitals, and specialty entities, there are specific steps to take and certain aspects to consider. As such, the Center for Health Care Strategies provided a brief detailing how to best develop an Accountable Care Organization (ACO) and support the facilities participating in the ACO.

First, it is necessary to develop care delivery innovations. Specifically, boosting primary care is vital when it comes to addressing patient needs and improving health outcomes. Additionally, in order to innovate in care delivery, population health management needs to be incorporated as well as strategies for care management with chronic medical conditions and general care coordination improvements.
Other broad goals set forth in the brief include strengthening data collection and quality of care. This includes reporting quality measures as well as focusing on data analysis and quality improvement strategies.
When developing an effective Accountable Care Organization, it is also vital to address patient engagement as well as propose community outreach efforts. In general, in order for an Accountable Care Organization to be successful, there will need to be strong leadership with a new vision and superior management skills.
The health payer’s role in ACO development
It is also vital to address the role of the health payer in the creation of the Accountable Care Organization. New payment models will need to be incorporated when a health payer teams up with an ACO to deliver high-quality care.
Most importantly, the health payer will need to contract with participating provider organizations and develop a system in which cost savings can be shared among all parties involved.
For instance, the Medicare Shared Savings Program sets up a certain reimbursement amount for each ACO and any costs that aren’t spent on medical services can then be shared among each party as long as the Accountable Care Organization met required performance quality measures.
An Accountable Care Organization often partners with Medicare, Medicaid, or a private insurer to better coordinate care and share in cost savings for meeting the quality improvement targets and healthcare cost reductions set forth in a contract. Additionally, sometimes an ACO could be penalized for not meeting a few requirements.
The Journal of the American Medical Association discussed one example in which a managed care contract and an Accountable Care Organization led to cost savings for the healthcare industry. Anthem Blue Cross in California became the health payer for a managed care system that included seven Los Angeles healthcare facilities. Both shared risk and savings were part of the contracted arrangement across all participating parties including the payer and the providers.
The costs of healthcare from both the payers’ and the providers’ seems to only steepen over the years, especially since the demand for healthcare coverage has increased tremendously since the Patient Protection and Affordable Care Act became the law of the land. As such, payers are more likely to move away from fee-for-service reimbursement and continue pursuing accountable care arrangements and bundled payments in order to put a dent in rising medical costs.
“Payment and incentives within an ACO should be structured to foster a shared sense of responsibility for both cost and quality. This provides an opportunity for a higher earning potential for physicians providing care in these ACOs,” the American Academy of Family Physicians reported.
“The idea of shared savings is that, by working together, a group of providers can deliver care at equal (or better) quality while reducing the cost below projections. There should be some savings to be shared between the payer– the government or the employer– and the providers.”
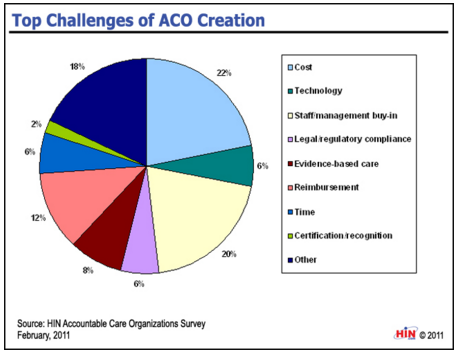
There are a number of challenges that must be addressed and solved when developing an Accountable Care Organization. This definitely includes managing reimbursement, costs, technology, and evidence-based care protocols. The graph below outlines the top obstacles that health payers and providers will need to consider when creating an accountable care arrangement.
The differences between private and public ACO contracts
When developing an accountable care arrangement, it is necessary to consider the details of partnering with either public or private payers. The Journal of the American Medical Association reported that contracts with a private payer tend to have more financial risk involved, which means providers will not be fully reimbursed when costs rise beyond the contracted amount.
However, when looking at the public sector, Medicare ACOs tend to be protected from this type of financial risk. Also, private payers tend to ensure there is a specific population of patients an ACO is responsible for. However, “Medicare ACOs are assigned beneficiaries retrospectively.”
Steps to support ACO participating providers
Health payers and state agencies will need to work with accountable care providers to understand their needs including any additional resources they may require. This could include mental health and behavioral health services, care coordination assistance, social service integration, or ways to improve health outcomes among low-income, Medicaid-based patient volumes.
Soliciting feedback and information from ACO providers will be key. This could lead states to build up the programs necessary to support more effective care coordination among multiple providers and hospitals.
“States can build more responsive programs by incorporating stakeholder feedback into the design of technical assistance,” The Center for Health Care Strategies stated in their brief. “Oregon held a pre-proposal conference before releasing an RFP to find a neutral convener that could lead practice technical assistance activities through its Patient-Centered Primary Care Institute. Oregon found that the public was very engaged during this process, identifying important considerations, and contributing to a stronger pool of applications.”
“Being transparent and open to public feedback has helped Oregon gain considerable buy-in from various parts of its health sector across many of its broad, statewide reform initiatives.”