How Payers Can Improve HEDIS Quality Measure Performance
Population health management, health IT investment, and provider engagement need to be targeted to improve HEDIS quality measure performance.

Source: Thinkstock
- HEDIS quality measures have a significant role in the healthcare industry regarding closing gaps in care and decreasing the use of costly acute care through preventive services. By placing a greater focus on value-based care and quality improvement across healthcare organizations, HEDIS quality measures hold a critical place in helping providers achieve these goals.
Health insurance companies have faced a number of challenges with improving their performance on HEDIS quality measures. These difficulties include the administrative burden of handling an excess of quality data, designing quality reporting scores, the lack of health IT adoption for reporting HEDIS scores among providers, and low preventive screening rates among their provider networks.
Health insurance companies have implemented best practices to overcome obstacles and improve their HEDIS quality scores. Payer solutions have included boosting population health management, creating a population health registry, and financially incentivizing physicians to adopt new technologies. Other best practices have focused on incorporating patient engagement, beneficiary incentive programs, cost transparency, and provider engagement.
Payers will need to integrate strong clinical documentation strategies, population health management, and provider engagement across their organization to succeed in improving the quality of care, raise HEDIS quality scores, and compete effectively in the health insurance market.
Dig Deeper:
Top 3 Ways to Meet HEDIS Quality Measures, Improve Performance
3 Key Steps for Health Payers to Meet HEDIS Quality Measures
What are HEDIS measures?
The Healthcare Effectiveness Data and Information Set (HEDIS) is a widely used group of measures that quantify quality performance among healthcare payers and providers in any given year. Some common HEDIS quality measures involve childhood immunization status, cancer screenings, asthma medication management, heart attack treatment, mental healthcare, flu shots, and high blood pressure treatment.
The National Committee for Quality Assurance (NCQA) is responsible for creating and defining HEDIS quality measures that make it possible for consumers to compare health plans and provider networks between different payers.
The 2017 HEDIS quality measures are divided up into five specific categories, which include (1) effectiveness of care, (2) access or availability of care, (3) experience of care, (4) utilization and relative resource use, and (5) health plan descriptive information. NCQA adds, deletes, and revises HEDIS measures on an annual basis.
NCQA collects HEDIS data using health insurance claims, surveys, and clinical documentation of hospitals, pharmacies, laboratories, and physician offices. The agency utilizes the Healthcare Organization Questionnaire as well as the Interactive Data Submission System to collect HEDIS data.
An NCQA-approved auditing firm then audits the data before reporting HEDIS quality measures publically. Once the results are available for public viewing, consumers may use the information to compare multiple health plans and local medical facilities.
Dig Deeper:
HEDIS Quality Performance Measures Assist Consumers, Insurers
NCQA Proposes New Changes to HEDIS Quality Measures in 2017
Biggest challenges of HEDIS quality reporting
In recent years, a large rise in the amount of healthcare quality data has hit the healthcare industry. The process of collecting and reporting on the data has led to low levels of physician satisfaction and higher physician burnout. A study from the Mayo Clinic and Cleveland State University shows that computerized physician order entry (CPOE) and electronic health record use led to higher rates of physician burnout.
Every year, big data is growing at a 48 percent rate and is expected to reach 2,314 Exabytes of data by 2020, according to a Dell EMC report. With more clinical information available, payers and providers have faced more complexities when attempting to measure and analyze healthcare data.
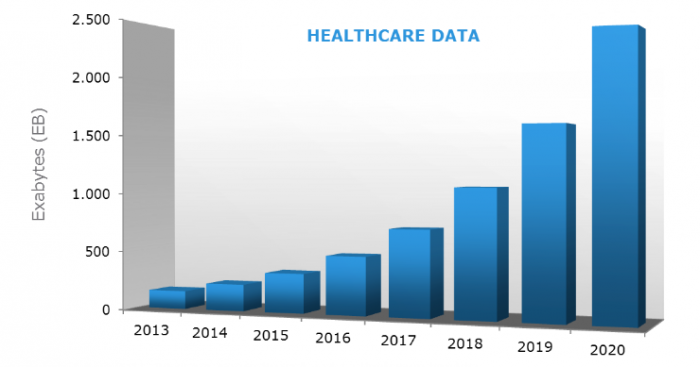
Source: EMC Digital Universe with Research & Analysis by IDC
Payers also face a lack of health IT adoption among providers, which may make it difficult to collect data required for HEDIS quality measures. Payers may need to assist providers in implementing the information systems required to support quality reporting and monitoring.
Some health insurers have also seen low preventive screening rates among their provider networks, which would inhibit them from raising their HEDIS scores. The National Cancer Institute and the Centers for Disease Control and Prevention found that screening for breast, colorectal, and cervical cancer are not meeting the benchmarks required by the disease prevention initiative Healthy People 2020 program. Rates of cervical cancer screening decreased in recent years while breast and colorectal screening remained stable.
While these are major challenges that payers have faced in attempting to improve HEDIS quality scores, health insurance companies and their provider networks have followed some best practices in overcoming these obstacles.
Dig Deeper:
Why HEDIS Quality Measures Matter for Value-Based Care
Payers Could Boost HEDIS Quality Measures by Exchanging Data
Best practices for improving HEDIS quality scores
Sponsors of HEDIS quality reporting must properly risk-adjust data so that adequate comparisons can be made between health plans and provider services. Adequate risk adjustment could enable consumers to compare health plans more fairly based on HEDIS quality scores.
However, many insurers have not properly aligned their risk adjustment and quality management. A report from Optum urges stakeholders to align quality management and risk adjustment in order to reduce healthcare spending, gain revenue growth, and improve patient outcomes.
When payers determine from the risk-adjusted data that changes in performance are tied largely to an organizational factor, it may be simpler to drive financial incentives or penalties to impact quality improvement. Payers could also use statistical analysis to determine whether any performance measures should be eliminated or changed.
To achieve higher HEDIS scores, providers will need to have accurate clinical documentation. Checking off which patient services were completed and which are still needed will help in identifying gaps in care as well as adhering to HEDIS quality measures.
Payers facing a lack of health IT investment from their provider networks could also improve documentation efforts through temporary staffing for reviewing and reporting HEDIS scores. For example, Blue Cross Blue Shield of Rhode Island hires temporary nursing staff each year to retrieve patient records, review the data, and enter information into a program holding HEDIS measures.
Population health management and patient data analytics could also help payers improve HEDIS quality scores. The first steps to take involve creating a population health registry and analyzing population health data.
Blue Cross Blue Shield of Rhode Island developed a population health registry in 2010. The payer adopted a cloud-based data analytics system to build a longitudinal disease registry, which includes six disease brackets, clinical measures, pay-for-performance information, and HEDIS quality measures. The population health registry helps Blue Cross Blue Shield of Rhode Island identify high-risk patients on a monthly basis.
The payer uses predictive analytics to forecast the spend of high-risk members. The data is entered into the population health registry and summaries are sent to primary care physicians and nurse care managers every month. Healthcare providers are then able to pursue outreach and engage with high-risk patients to reduce overall healthcare use and high rates of medical spending.
Patient outreach and engagement is expected to play a role in improving HEDIS scores by involving patients in clinical decision-making. Patients who are engaged and taking part in provider conversations about their health should have better outcomes since these patients are more likely to take part in preventive care and primary care visits.
Payers will need to incorporate patient engagement in their clinical quality measures and financial incentives in order to ensure patient outreach is achieved. To meet HEDIS quality benchmarks regarding patient health outcomes, payers and providers will need to invest in patient engagement.
To improve engagement and wellness among the patient community, payers should incorporate beneficiary incentive programs. Beneficiary incentive programs offer economic incentives to health plan members who exhibit healthy lifestyle choices such as a gym membership. For example, some state Medicaid programs have included incentives in the form of gift cards, cash, meals, childcare, or transportation.
The Affordable Care Act has enabled state Medicaid programs to apply for grants that would provide incentives for Medicaid beneficiaries who have shown healthy behaviors. A state Medicaid program must focus on key goals when applying for these beneficiary incentive grants.
These goals include reducing the rates of smoking, improving weight management and diabetes management, and decreasing cholesterol and blood pressure rates. Since these goals align with HEDIS scores, payers will be able to reach higher clinical quality measures. Commercial payers can follow in the footsteps of state Medicaid programs and implement member incentives.

Dr. Thomas Mackey, PhD.
Payers will need to focus on provider engagement since these are the professionals in charge of managing HEDIS quality scores and patient outcomes. Provider engagement should also increase rates of preventive screening, said Dr. Thomas Mackey, PhD., a Nurse Practitioner from the University of Texas Health Services.
Mackey explained that engaging medical teams at physician practices is key in improving HEDIS quality scores. Front desk staff and nurse practitioners will all need to coordinate care to improve preventive screening among their patient base.
“The number one thing I would suggest is to make sure your staff is engaged,” Mackey said. “The challenges have to do with getting the practice and the people in that practice - I don’t mean just the physicians or the nurse practitioners but I mean the front desk as well as the nurses in the back - to help meet the HEDIS measures when a patient comes in.”
“If we’re talking about colorectal cancer screening, when a patient comes in for a health maintenance visit or a respiratory infection and we might not see them for a year or two years, [we need] to try and get some of the HEDIS measures met for that patient,” Mackey urged.
By following these best practices, health insurers are likely to increase their HEDIS quality scores across their health plans and provider networks.
Dig Deeper:
Key Ways Blue Cross Blue Shield Raises its HEDIS Scores
Best Practices to Drive HEDIS Success in 2017
Key factors for raising HEDIS scores
Health insurance companies have faced a number of challenges reporting and improving HEDIS quality measures including the administrative burden of an excess of quality data, the complexity of data analysis, and adopting health IT platforms for reporting HEDIS scores.
In order to improve HEDIS quality scores, health payers will need to focus on improving healthcare documentation and adopting new health IT solutions, increasing preventive screening rates, population health management, patient and provider engagement, and transitioning reimbursement contracts to value-based care payment models.
Public and private payers are expanding value-based care reimbursement, which is expected to improve quality, close gaps in care, and, thereby, help payers achieve higher HEDIS scores. Following these steps should help commercial payers achieve their goals in improving their performance on HEDIS quality measures.
Dig Deeper:
Top 3 Ways to Meet HEDIS Quality Measures, Improve Performance
3 Key Steps for Health Payers to Meet HEDIS Quality Measures
