Gallup Reports 4-Year High in Number of Uninsured Americans
The percentage of uninsured Americans is on the rise with women, young adults, and lower-income individuals representing the largest increases.

Source: Thinkstock
- Earlier this week, the Gallup National Health and Well-Being Index reported that the percentage of adults without health insurance reached 13.7 percent by the close of 2018. The polling group sampled more than 115,000 adults across the country.
The latest increase continues an upward trend since the third-quarter of 2016 when the rate of uninsured Americans dipped to 10.9 percent, down from a high of 18.0 percent prior to the opening of ACA exchanges in 2013.
While the uninsured rate grew across the board for all populations, the most significant areas of growth were among women, young adults, and lower-income individuals. Specifically, Gallup researchers honed in on differences in uninsured rates between the final quarter of 2016 and 2018.
During that two-year period, the percentage of uninsured women rose from 8.9 percent to 12.8 percent, a 3.9-percent change compared to a 1.6-percent increase for men.
Among Americans ages 18 to 34, the uninsured rate jumped from 16.8 percent in 2016 to 21.6 percent, nearly 8 percentage points higher than 35-64 (13.7%) and 7 times higher than 65+ (3.7%).
For households with income less than $24,000, the uninsured rate rose to 25.4 percent from 22.6 percent just two years prior. A similar uptick emerged among households with an annual income between $24,000 and $48,000 — 16.1 percent up to 19.1 percent.
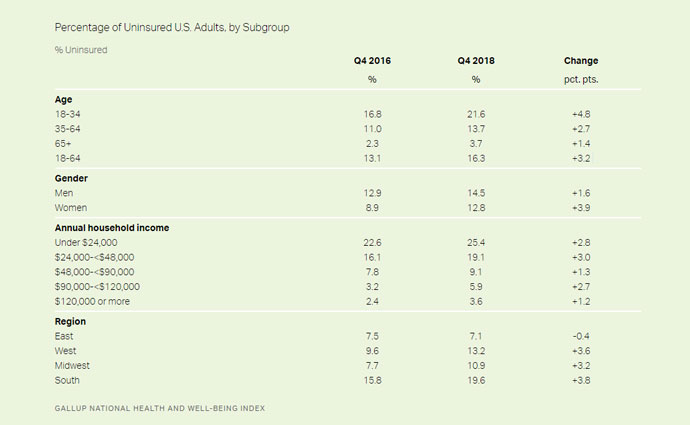
Source: Gallup
Geographically, an upsurge in the uninsured rate was common for all regions except the East, which actually saw a drop from 7.5 percent to 7.1 percent. Conversely, the geography with the largest percentage of uninsured Americans, the South, experienced a 3.8-percent increase, followed by 3.6-percent and 3.2-percent increases in the West and Midwest, respectively.
Gallup list a number of factors that have contributed to the national rise in the uninsured rate. The first is the increased cost of health insurance premiums.
“For enrollees with incomes that do not qualify for government subsidies, the resulting hike in rates could have had the effect of driving them out of the marketplace. Insurers have also increasingly withdrawn from the ACA exchanges altogether, resulting in fewer choices and less competition in many states,” writes Dan Witters.
Other factors stem from the battle playing out in Washington, DC, between Democrats and Republicans.
The Trump Administration has made its dissatisfaction with the ACA exchanges well known.
“The open enrollment periods since 2018 have been characterized by a significant reduction in public marketing and shortened enrollment periods of under seven weeks, about half of previous periods,” Witters notes.
“Funding for ACA ‘navigators’ who assist consumers in ACA enrollment has also been reduced in 2018 to $10 million, compared with $63 million in 2016,” he continues. “Overall, after open enrollment in the ACA federal insurance marketplace (i.e., healthcare.gov) peaked in 2016 at 9.6 million consumers, it declined by approximately 12.5%, to 8.4 million in 2019, based on recently released figures.”
The elimination of the individual mandate was also a contributing factor, according to Gallup.
For lower-income individuals, the end of cost sharing likely contributed to a decline in insured adults.
“The cost-sharing payments were made to insurers in the marketplace exchanges to offset some of their costs for offering lower-cost plans to lower-income Americans,” concludes Witters. “The Trump administration had previously renewed the payments on a month-by-month basis but later concluded that such payments were unlawful. In April 2018, a federal court granted a request for a class-action lawsuit by health insurers to sue the federal government for failing to make the payments. Such lawsuits continue to be litigated.”
Should regulatory and legal uncertainty remain, the ACA’s positive impact on driving down the uninsured rate is likely to be offset.
