GAO: Erroneous Medicaid Claims Data Pose Fraud Risk at CMS
Personal care services for Medicaid beneficiaries are at high risk for fraud because of missing, siloed, and inaccurate Medicaid claims data in a pair of CMS systems.

Source: Thinkstock
- Millions of people rely on long-term personal care services under Medicaid coverage, but significant gaps and errors in two major CMS data systems are creating significant opportunities for fraud and abuse.
A new report from the Government Accountability Office (GAO) found more than $4.9 billion in misidentified Medicaid claims through 2012 along with noteworthy shortcomings in data integrity and Medicaid claims data reporting.
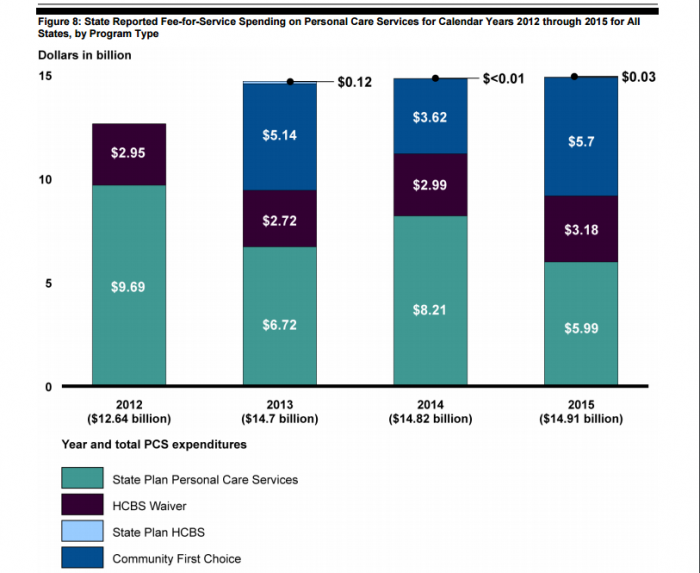
Medicaid spending on home health and personal care services has grown in recent years due in part to a focus on keeping patients out of the hospital and in the home. The program’s long-term personal care budget eclipsed $80 billion in the year 2014 and is expected to grow to $111 billion by the year 2026, according to the report.
But the relative ease of establishing a home health service, as well as lackluster enforcement of data reporting requirements, make CMS programs vulnerable to fraudulent claims.
Over the past few years, CMS has taken several actions to combat fraud in Medicare and Medicaid, including a program that required certain home health agencies to undergo a pre-claims review before they could receive reimbursement through Medicare.
Fraud is such a problem for CMS that the federal agency went as far as targeting six states known to frequently submit fraudulent claims, and ended up blocking enrollment in CMS programs. Through these and other fraud prevention and detection activities, CMS has been able to save $42 billion.
But GAO believes that CMS could be doing more to limit fraudulent claims and keep track of participating providers, starting with an overhaul of the agency’s two main reporting systems: the Medicaid Statistical Information System (MSIS) and the Medicaid Budget and Expenditure System (MBES).
In 2012, which was the most recent dataset available to investigators, only 35 states reported claims at all. Twenty percent of those claims were missing payment amounts. Thirty-four percent had missing quantity of service numbers.
“The usefulness of the data collected from these two systems for CMS oversight is limited because of data gaps and errors,” GAO reported. “To provide effective oversight, including decision making, external reporting, and monitoring program operations, CMS needs timely, relevant and reliable data on personal care services rendered and the amount paid. GAO found that the data collected did not always meet these standards.”
Source: GAO
MSIS data also lacked provider identification numbers for 15 percent of claims. Claimants used more than 400 procedure codes to identify the services of these claims, with large variations between time period and quantity.
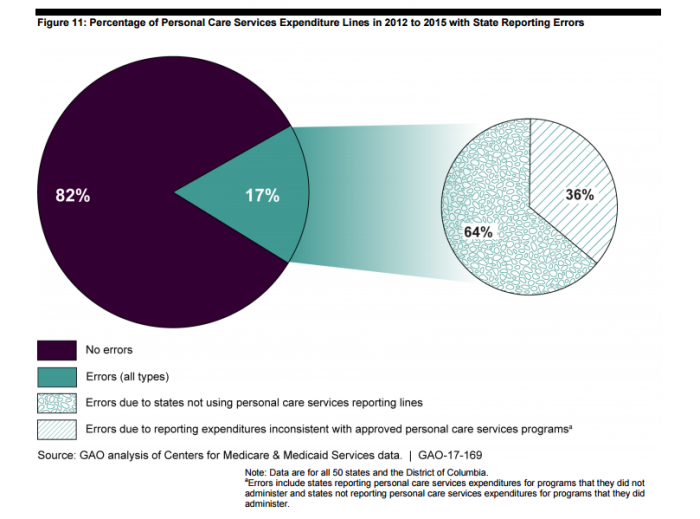
The second data system, MBES, collects aggregate expenditures of states across 80 service categories. From 2012 to 2015, 17 percent of expenditure lines were reported incorrectly to MBES. Two-thirds of these errors resulted from states not separating identifying personal care expenditures, a CMS requirement.
Source: GAO
CMS currently is looking for a replacement for MSIS and has established an office dedicated to data monitoring. GAO, however, advised that CMS needs to establish proper data standardization before those initiatives become effective.
“GAO recommends that CMS improve personal care services data by: establishing standard reporting guidance for key data; ensuring linkage between data on the provision of services and reported expenditures; ensuring state compliance with reporting requirements; and developing plans to use data for oversight.”
Upon review of the report, HHS agreed that CMS must better ensure that states comply with reporting requirements and should build better ways to analyze and use data. HHS did not explicitly agree with ensuring linkage between provision of personal care services and reporting expenditures.
