Prescription Drugs Account for 22% of Payer Premium Spending
New research has found that prescription drug costs and physician services are the largest parts of healthcare premium dollars.
Source: Thinkstock
- Prescription drug costs consume the largest proportion of dollars spent on healthcare premiums, with 22 cents out of every dollar going to medication costs, says AHIP in a new data brief.
Eighty percent of every dollar is spent on medical expenses, and the remaining 20 percent was split between operating costs and net margins, showing that payers are adhering to the 80/20 rule instituted by the ACA.
“This is the latest evidence that shows prescription drug costs are out of control,” said Marilyn Tavenner, President and CEO of AHIP in an accompanying statement.
“The vast majority of every dollar spent by consumers on insurance premiums is returned in direct medical services, including prescription drugs. That’s why we need real solutions that answer the President’s call to ‘bring down the artificially high price of drugs’ so that consumers can affordably get the care they need.”
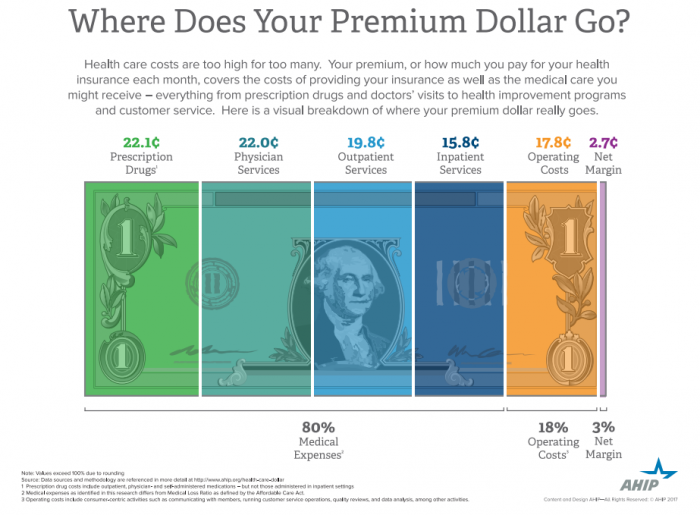
Source: AHIP
The AHIP report used data from premiums contributed by patients under 65 who were continuously insured.
Outpatient services consumed 19.8 cents of every dollar while 15.8 cents were spent on covering inpatient services. Operating costs for payers were 17.8 cents per premium dollar.
In 2014, healthcare expenses totaled $104 billion. Prescription drug spending accounted for $28.9 billion and physician services accounted for $28.8 billion. Outpatient and inpatient services, respectively, cost $26.1 and $20.7 billion.
Prescription drugs are costly to both consumers and healthcare providers. Last year, CMS beneficiaries were subject to paying extremely high prices for specialty drugs, with totals consumer expenses on drugs ranging from $600 to over $37,000.
Earlier this year, the Association of Cancer Care Centers (ACCC) named prescription drug costs among some of the top challenges for providing care according to an ACCC survey. HRSA even created a $5,000 fine for drug companies that intentionally charge hospitals higher-than-average celing prices for 340B drugs.
Prescription drug spending can also be impeded by administrative challenges, as evidenced by the Wisconsin’s state government improperly claiming over $3 million in Medicaid drug reimbursement.
